Call: (702) 388-8979
Request AppointmentBlog
July 21, 2016

The number of aging patients at dental offices has been steadily increasing in recent years. At the same time, seniors are keeping their natural teeth longer and fewer patients are wearing dentures. Because the senior population will continue to swell as baby boomers reach the age of retirement, dental professionals are adapting their practices to meet the needs of older patients.
Dentists must take into account the reduced mobility and dexterity of some seniors, which may make routine oral hygiene practices difficult. Your existing medical conditions and treatments are also an important factor in determining dental care.
You may be unfamiliar with current dental practices and choose not to seek dental care for dental problems like toothache remedies, bleeding gums and improperly fitted dentures, but it's important that you do. There are many dental technologies now available to help make dental treatment of common problems more comfortable and less time-consuming.
Your oral health is an important component of your overall health, so it's even more important for you to visit the dentist regularly and maintain good dental health as you age. Because tooth decay is more likely to occur in older adults, it is important to brush and floss regularly to remove dental plaque that could cause periodontal disease, thus reducing the possibility of needing costly gum disease treatment.
Using fluoride is one of the most effective ways to strengthen teeth and prevent harmful acids from causing tooth decay: It promotes the absorption of calcium and phosphorus into the tooth enamel, which helps to repairs weak spots. Most towns and cities have fluoridated tap water, which provides an adequate source of fluoride. If your tap water is not fluoridated, speak with your dentist about other sources of fluoride.
December 30, 2015

May 9, 2015
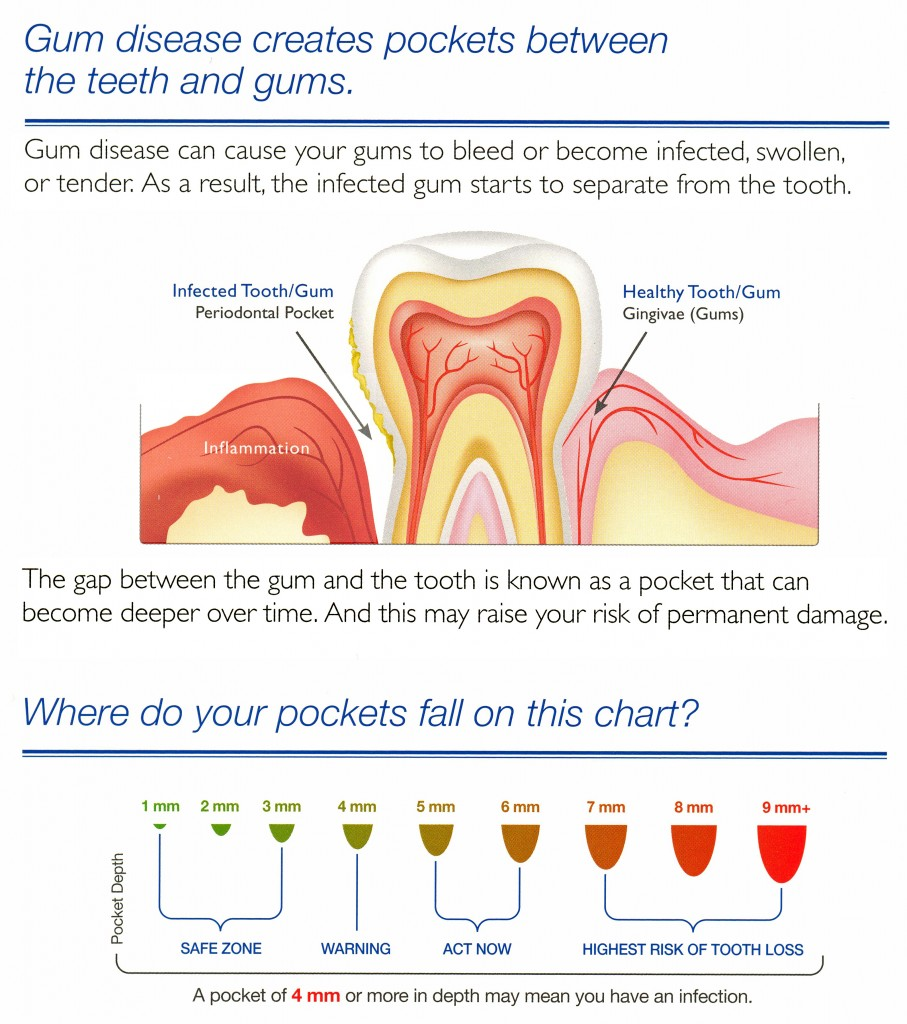
When you see me as a new patient for an initial examination or when you visit our hygienists to get your teeth cleaned you will have the health of your gums evaluated by using a simple and relatively painless test called a periodontal chart or periochart. Most likely you will hear our hygienist calling out a series of 6 numbers per tooth.What we are doing is measuring, in millimeters (mm), the depth of the cuff of gum tissue around each tooth.This depth is the difference in height between the level of your gumline and the point at which the gum actually attaches to your tooth. 2-3 mm is considered healthy and physiologic and anything over 5 mm usually indicates that the bone that supports your tooth has begun to be destroyed by disease. The diagram at the top of the blog explains it better, but here is a little more detail on what measuring the “pockets” mean:
0 to 3 mm without bleeding: Congratulations! No issues!
1 to 3 mm with bleeding: This is gingivitis which is the mildest form of gum disease. Usually a good cleaning coupled with improved oral self-care is all that is needed.
3 to 5 mm with no bleeding: There is a strong potential of gum disease. Routine cleanings cannot reliably go deeper than 3 mm. Three to four visits a year may be recommended to improve the situation.
3 to 5 mm with bleeding: Early to moderate gum disease (beginning Periodontitis) which may require some additional treatment as well as better home care and three to four visits per year.
5 to 7 mm with bleeding: Bone loss is likely as is soft and hard tissue damage. Almost always requires definitive treatment, possibly over several visits, as well as greatly improved home care andthree to four hygiene visits per year to prevent tooth loss.
7mm and above with bleeding: Advanced periodontal disease which means aggressive treatment to save your teeth.Additionally, surgery is almost always required to repair the damage done.Periodontal maintenance visits are also required every 3-4 months thereafter.
As noted, the presence of bleeding or pus when you are being periocharted is a strong indicator of disease. Healthy gums do not bleed! The presence of gum disease leads to tooth loss and a greatly diminished quality of life. Gum disease is also implicated in serious health issues such as heart disease and strokes, diabetes, and respiratory problems.
So, don’t put it off! Contact me or my excellent staff at 702-388-8979 for a periodontal (gum) evaluation. The earlier these problems are detected, the easier and more predictable thetreatment is.
_______________________________________________________________________________
March 23, 2015
The Importance of Fluoride

Fluoride is a mineral that occurs naturally in many foods and water. Every day, minerals are added to and lost from a tooth's enamel layer through two processes, demineralization and remineralization. Minerals are lost (demineralization) from a tooth's enamel layer when acids -- formed from plaque bacteria and sugars in the mouth -- attack the enamel. Minerals such as fluoride, calcium, and phosphate are redeposited (remineralization) to the enamel layer from the foods and waters consumed. Too much demineralization without enough remineralization to repair the enamel layer leads to tooth decay.
Fluoride helps prevent tooth decay by making the tooth more resistant to acid attacks from plaque bacteria and sugars in the mouth. It also reverses early decay. In children under 6 years of age, fluoride becomes incorporated into the development of permanent teeth, making it difficult for acids to demineralize the teeth. Fluoride also helps speed remineralization as well as disrupts acid production in already erupted teeth of both children and adults.
A dentist in his or her office can apply fluoride to the teeth as a gel, foam, or varnish. These treatments contain a much higher level of fluoride than the amount found in toothpastes and mouth rinses. Varnishes are painted on the teeth; foams are put into a mouth guard, which is applied to the teeth for one to four minutes; gels can be painted on or applied via a mouth guard.
It is certainly important for infants and children between the ages of 6 months and 16 years to be exposed to fluoride. This is the time frame during which the primary and permanent teeth come in. However, adults benefit from fluoride, too. New research indicates that topical fluoride -- from toothpastes, mouth rinses, and fluoride treatments -- are as important in fighting tooth decay as in strengthening developing teeth.
In addition, people with certain conditions may be at increased risk of tooth decay and would therefore benefit from additional fluoride treatment. They include people with:
- Dry mouth conditions: Also called xerostomia, dry mouth caused by diseases such as Sjögren's syndrome, certain medications (such as allergy medications, anti-histamines, anti-anxiety drugs, and high blood pressure drugs), and head and neck radiation treatment makes someone more prone to tooth decay. The lack of saliva makes it harder for food particles to be washed away and acids to be neutralized.
- Gum disease: Gum disease, also called periodontitis, can expose more of your tooth and tooth roots to bacteria increasing the chance of tooth decay. Gingivitis is an early stage of periodontitis.
- History of frequent cavities: If you have one cavity every year or every other year, you will benefit from additional fluoride.
- Presence of crowns and/or bridges or braces: Decay often appear at the point where the crown meets the underlying tooth structure or around the brackets of orthodontic appliances.
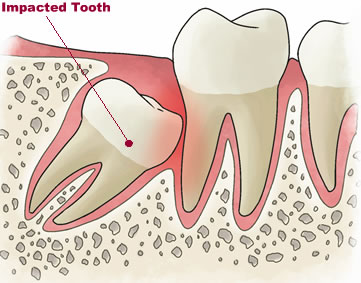
A tooth is considered impacted when it only partially grows through the gums. This can happen because another tooth blocks it, or it grows in crookedly. The third molar typically erupts from age 17 to 21 and is the last tooth to appear, which is why it’s the most likely tooth to become impacted – there’s usually no room left for it.
